What is a Cavity? Edina Dentist Explains
What is a cavity? Learn how to prevent one and treatment options
Cavities are a common occurrence worldwide. In the US alone, more than half (57%) of adolescents aged 12 to 19 have had a cavity in their permanent teeth. Among adults aged 20 and older, about 90% have had at least one cavity. But what is a cavity exactly? Can they be prevented (yes!)? And what is the treatment? We’ll tell you all you need to know about cavities, also known as dental caries.
In This Article:
What is a cavity?
A cavity, scientifically named dental caries, is essentially a hole in a tooth. This hole is caused by the gradual erosion of its hard outer layer, enamel. It’s a common dental issue, affecting individuals of all ages. Sugary food, bacteria in your mouth, or soda are common instigators of cavities. Let’s dive in.
The bad guys causing dental caries
Our mouths are bustling with all sorts of bacteria – some good, some bad. The troublemakers join forces and cause tooth decay. It happens when certain bacteria feast on sugars in our food, creating acids that slowly dig holes in our teeth.
Smooth surface cavities slowly dissolve enamel, often appearing between teeth. Pit and fissure decay target the top surface of chewing areas, progressing rapidly. Root decay poses challenges, primarily impacting adults with receding gums, as exposed roots become vulnerable to plaque and acid.
Your mouth has some natural resistance. Minerals in saliva and fluoride assist in repairing enamel during these acid attacks.

Five stages of decay
Understanding the five main stages of tooth decay provides insight into the progression:
- Demineralization
In this initial stage, you may observe small, white, chalky spots on your tooth. This indicates the breakdown of minerals in your tooth enamel. - Enamel decay
If left untreated, tooth decay advances, further breaking down the enamel. Cavities, or noticeable holes, may become apparent. White spots may evolve into a light brownish color. - Dentin decay
Dentin, situated just beneath the enamel, is softer. Plaque and bacteria reaching this layer accelerate cavity formation. Teeth sensitivity becomes noticeable, and the spots on your teeth may darken to a deeper brown. - Pulp damage
The tooth pulp, the innermost layer containing nerves and blood vessels, becomes compromised. Cavities reaching this stage result in pain, along with redness and swelling in the surrounding gums. The spots on your tooth may transition to a darker brown or black. - Abscessed tooth
When left untreated, a deep cavity can lead to infection, forming a pocket of pus at the tooth root’s tip (periapical abscess). Symptoms may include radiating pain, facial swelling, and swollen lymph nodes. If left unaddressed, a tooth abscess can potentially spread to surrounding tissues, other body areas, or, in rare and extreme cases, to the brain or bloodstream (sepsis).
Causes of tooth cavities
Tooth cavities are sparked by plaque, a sticky mix of bacteria, saliva, acid, and food particles that cling to your teeth. After eating sugary treats, bacteria in your mouth get to work, turning sugar into acid. This acid starts forming plaque on your teeth, making regular brushing crucial.
When plaque is not removed, it causes eroding of the hard enamel coating that shields your teeth from decay. Back teeth are cavity prone, due to their tricky-to-reach nature and uneven surfaces that trap food.
Multiple players cause cavities. In this order, these are some main troublemakers:
- Bacteria and sweets
Sugary and starchy foods become a feast for bacteria in your mouth, turning them into acids. - Plaque
A sticky film called dental plaque forms on your teeth, blending bacteria, acid, food, and saliva. - Enamel erosion
Without diligent brushing and flossing, the acids in plaque start dissolving tooth enamel, creating those notorious cavities.
Risk factors for cavities
Certain things make you more likely to get cavities. If your mouth is often dry, maybe because of a health condition or certain medicines, you’re at a higher risk. Eating lots of sugary or starchy foods, or snacking all the time, also makes cavities more likely.
A family history of cavities can amplify your likelihood of experiencing them. Furthermore, as gums recede, exposing tooth roots, the risk of cavities intensifies.
While cavities themselves aren’t contagious, the bacteria responsible can jump from one person to another. A kiss can theoretically transfer them, for example.
Symptoms of a cavity
Detecting a cavity isn’t always straightforward, especially in the early stages when it lurks on the outer enamel without causing pain. However, as decay digs deeper into the dentin and pulp, symptoms may emerge.
Unpleasant signs
- Bad breath or a lingering bad taste in your mouth.
- Bleeding gums or indications of gum disease.
- Facial swelling, hinting at underlying dental issues.
- Toothache or general mouth pain.
- Tooth sensitivity, especially to hot or cold foods and drinks.
Varied indications of decay
The severity of cavity symptoms varies, ranging from subtle signs to more pronounced issues.
Sensitivity signals
- Tooth sensitivity, a common early sign of enamel erosion.
- Tooth pain, an indication that decay has progressed.
Visible clues
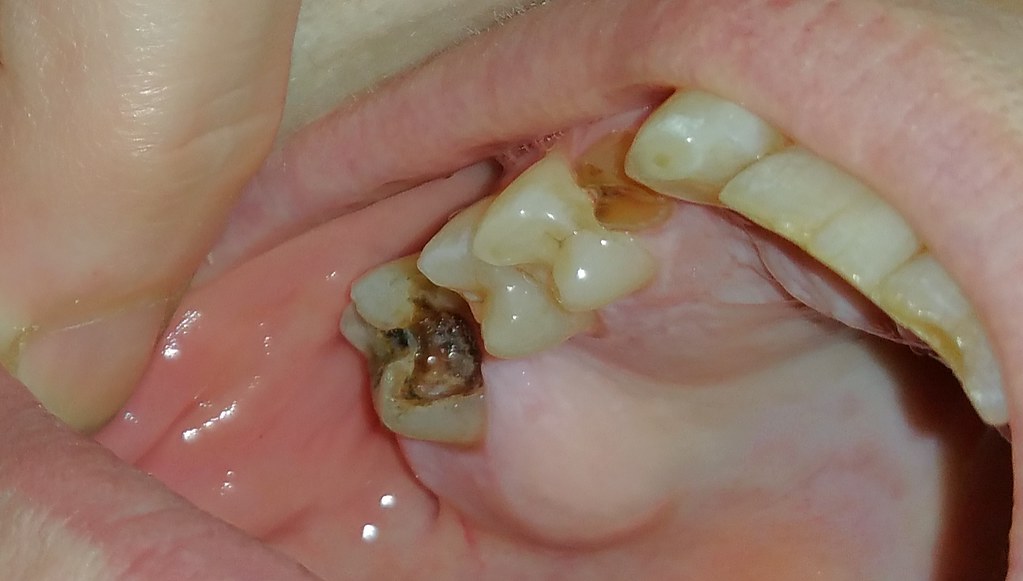
- A visible hole in the affected tooth, marking the advance of decay.
- Black or white staining on the tooth’s surface, revealing the impact of cavities.
Progressive symptoms
- Toothache and persistent pain as the cavity expands.
- Sensitivity intensifies, causing discomfort with sweet, hot, or cold substances.
- Noticeable holes or pits in the teeth.
- Discoloration, with brown, black, or white stains appearing on the tooth surface.
- Pain during biting or chewing, signaling advanced decay.
What can we do about cavities?
The approach to treating tooth cavities is contingent upon the severity of the decay. For less extensive cavities, dental fillings are a common remedy. The dentist uses a drill to remove the decayed material and subsequently fills the tooth with a chosen substance, which may include silver, gold, or composite resin.
In cases of more advanced decay, dental crowns come into play. Custom-fit caps are placed over the tooth to replace its natural crown, necessitating the removal of decayed tooth material prior to the procedure.
For instances where decay has reached the nerves, a root canal becomes a viable solution. We take out the nerve and blood vessels, clean up the bad parts, and put medicine in there. After that, we fill up the tooth, and sometimes, we put a crown on top to make it stronger.
When we catch cavities early on, we can use fluoride treatments. They serve to restore tooth enamel and halt further decay, offering a proactive measure to preserve dental health.
Mint dental helps prevent cavities
When it comes to cavity management, our skilled dentists employ a range of effective strategies.
Preventive measures are most important. Regular dental check-ups and cleanings are crucial, allowing us to detect cavities in their early stages. Through thorough examinations, we identify potential issues, offering timely intervention before cavities escalate.
Proper maintenance, before or after a cavity treatment, is essential. We give you insights into proper oral hygiene practices and dietary choices, minimizing the risk of future cavities. We strive to equip you with the tools needed for long-term oral health.

